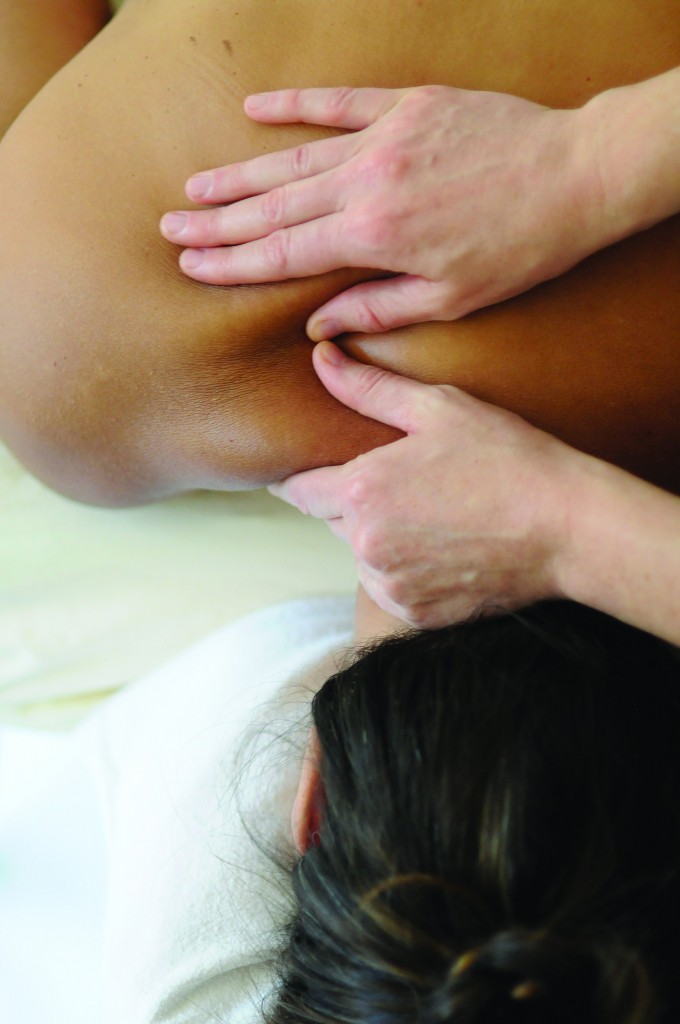
Swedish Massage—The most common form of massage. The Swedish technique mainly relaxes the muscles and eases aches and pains.
Tag Archives: pain
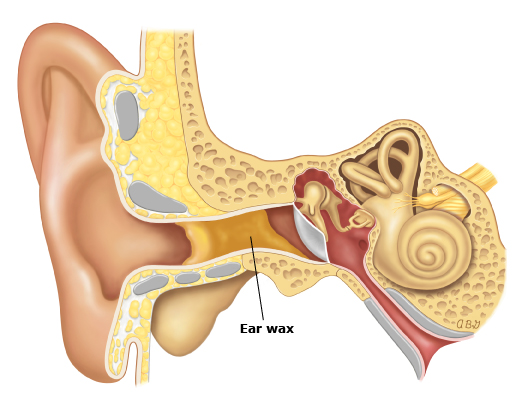
Impacted Ear Wax
Earwax is produced by glands in the ear canal. Although scientists are still not completely sure why we have earwax, its purpose is to trap dust and other small particles and prevent them from reaching, and potentially damaging or infecting the eardrum.
Symptoms of an earwax impaction include:
Decreased hearing
Dizziness
Ear pain
Plugged or fullness sensation
Ringing in the ear
Itching or drainage from the ear canal
See your doctor if you think you may have any symptoms of an earwax impaction. Other conditions may cause these symptoms and it is important to be sure earwax is the culprit before trying any home remedies.
Scoliosis
Health reasons why massage should be included in every person’s budget and schedules
Clergyman’s Knee
The knee is one of the largest and most complex joints in the body.
Clergyman’s knee or bursitis is caused by kneeling for long periods of time or repetitive knee movements. Fluid builds up in the bursa, the sac of fluid that cushions the knee joints. Swelling behind the knee is called a ‘Baker’s cyst’ and may be caused by injuries or arthritis.
Treatment of Bursitis or Clergyman’s Knee of not infected:
•Rest.
•Direct pressure on the knee should be avoided such as when kneeling.
•Cold therapy helps in reducing the pain and swelling.
•Compression helps in reducing the pain and swelling.
•Advanced massage therapy techniques can also be employed to help with the inflammatory process.
Please note!
A compression bandage is not suggested because compression would create more friction around the joint.
Are your employees stressed?
From manufacturers to hospitals to auto dealerships, companies across the country are using seated massage services to make work less of a pain in the neck for employees. Chair massage provides hard-working employees with a convenient method of alleviating the stress inherent in these competitive times.
Provide a unique benefit for your employees with Monica.
How will I feel?
After a massage with Monica Bemus most people feel very relaxed. Some experience freedom from long-term aches and pains developed from tension or repetitive activity. After an initial period of feeling slowed down, people often experience increased energy, heightened awareness, and greater productivity, which can last for days. Since toxins are released from your soft tissues during a massage, it is recommended you drink plenty of water afterward.
Dehydration
Dehydration occurs when your body loses too much fluid. This can happen when you stop drinking water or lose large amounts of fluid through diarrhea, vomiting, sweating, or exercise. Not drinking enough fluids can cause muscle cramps. You may feel faint. Usually your body can reabsorb fluid from your blood and other body tissues. But by the time you become severely dehydrated, you no longer have enough fluid in your body to get blood to your organs, and you may go into shock, which is a life-threatening condition.
Dehydration can occur in anyone of any age, but it is most dangerous for babies, small children, and older adults.
Babies and small children have an increased chance of becoming dehydrated because:
• A greater portion of their bodies is made of water.
• Children have a high metabolic rate, so their bodies use more water.
• A child’s kidneys do not conserve water as well as an adult’s kidneys .
• A child’s natural defense system that helps fight infection (immune system) is not fully developed, which increases the chance of getting an illness that causes vomiting and diarrhea.
• Children often will not drink or eat when they are not feeling well.
• They depend on their caregivers to provide them with food and fluids.
Dehydration in older adults
Older adults have an increased chance of becoming dehydrated because they may:
• Not drink because they do not feel as thirsty as younger people.
• Have kidneys that do not work well.
• Choose not to drink because of the inability to control their bladders (incontinence).
Have physical problems or a disease which makes it:
• Hard to drink or hold a glass.
• Painful to get up from a chair.
• Painful or exhausting to go to the bathroom.
• Hard to talk or communicate to someone about their symptoms.
• Take medicines that increase urine output.
• Not have enough money to adequately feed themselves.
Watch babies, small children, and older adults closely for the early symptoms of dehydration anytime they have illnesses that cause high fever, vomiting, or diarrhea. These are the early symptoms of dehydration:
• The mouth and eyes may be drier than usual.
• The urine may be darker than usual.
• The person may feel cranky, tired, or dizzy.
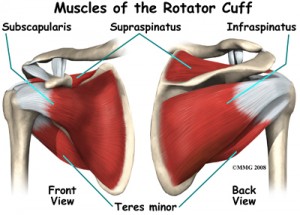
Rotator Cuff Injury & Tears
It’s one of the darkest fears of pitchers, tennis players, and many other athletes: a rotator cuff tear. If it is severe, a rotator cuff tear can end a player’s career. So what is it, exactly?
The rotator cuff is a group of four tendons and muscles that converge around the shoulder joint at the top of the humerus, the upper arm bone above the elbow. Together, they form a ”cuff” that both holds your arm in place and allows it to move in different directions. While your shoulder is one of your most mobile joints, it’s also somewhat weak. Too much stress — or too many fastballs — can cause partial tears and swelling in the tendons of the rotator cuff. Abrupt stress may even cause one of the tendons to pull away from the bone or tear in the middle of the tendon. Rotator cuff tears are sometimes incorrectly called ”rotary cuff tears.”
Athletes prone to getting rotator cuff tears include:
•Baseball players, especially pitchers
•Swimmers
•Tennis players
•Football players
You can get a rotator cuff tear by:
•Falling on your shoulder
•Using an arm to break a fall
•Lifting heavy weights
What Are the Symptoms of a Rotator Cuff Tear?
The symptoms of a rotator cuff tear include:
• Pain in the shoulder and arm, which varies depending on how serious the tear is
• Weakness and tenderness in the shoulder
•Difficulty moving the shoulder, especially when trying to lift your arm above your head
•Snapping or crackling sounds when moving the shoulder
•Inability to sleep on the shoulder
Most rotator cuff tears develop gradually. But they also can happen suddenly — you might feel a pop, intense pain, and weakness in the arm.
To diagnose a rotator cuff tear, your doctor might want to order the following tests:
•X-ray of the shoulder with some special views
• MRI (Magnetic Resonance Imaging)
• Arthrogram, a special type of X-ray or MRI done after a dye is injected into joint; this will allow your doctor to see more detail.
• Arthroscopy, a minimally invasive surgical procedure in which a tiny camera is inserted into the shoulder joint to get a look at the rotator cuff Arthroscopy is usually not done unless it is likely that you will need a surgical repair based on the other non-surgical tests.
These tests will allow your doctor to rule out other conditions and confirm that you have a rotator cuff tear. He or she may refer you to an orthopedic surgeon for treatment.
What’s the Treatment for a Rotator Cuff Tear?
As bad as these injuries can be, the good news is that many rotator cuff tears heal on their own. You just need to give them a little time. You also should:
• Rest the joint as much as possible. Avoid any movement or activity that hurts. You may need a sling.
• Ice your shoulder two to three times a day to reduce pain and swelling.
•Perform range-of-motion exercises
•Consider physical therapy to strengthen the joint.
More serious rotator cuff tears require surgery. One procedure is shoulder arthroscopy, usually an outpatient procedure. During an arthroscopy, the patient is put to sleep with general anesthesia. A small camera is inserted into the shoulder to see and repair the rotator cuff tear. If the tear is very large or involves more than one tendon, a small incision may be needed. Following arthroscopy, the arm will likely be in a sling for two to three weeks and physical therapy will be prescribed.
Turf Toe!
Turf toe is not a term you want to use when talking to a head football coach about his star running back or the ballerina before her diva debut. “Turf toe” is the common term used to describe a sprain of the ligaments around the big toe joint. Although it’s commonly associated with football players who play on artificial turf, it affects athletes in other sports including soccer, basketball, wrestling, gymnastics, and dance. It’s a condition that’s caused by jamming the big toe or repeatedly pushing off the big toe forcefully as in running and jumping.
Here is information about turf toe — what causes it, how to prevent it, and how it’s treated — to help you stay in the game.
What Causes Turf Toe?
Turf toe is a sprain to the ligaments around the big toe joint, which works primarily as a hinge to permit up and down motion. Just behind the big toe joint in the ball of your foot are two pea-shaped bones embedded in the tendon that moves your big toe. Called sesamoids, these bones work like a pulley for the tendon and provide leverage when you walk or run. They also absorb the weight that presses on the ball of the foot.
When you are walking or running, you start each subsequent step by raising your heel and letting your body weight come forward onto the ball of your foot. At a certain point you propel yourself forward by “pushing off” of your big toe and allowing your weight to shift to the other foot. If the toe for some reason stays flat on the ground and doesn’t lift to push off, you run the risk of suddenly injuring the area around the joint. Or if you are tackled or fall forward and the toe stays flat, the effect is the same as if you were sitting and bending your big toe back by hand beyond its normal limit, causing hyperextension of the toe. That hyperextension, repeated over time or with enough sudden force, can — cause a sprain in the ligaments that surround the joint.
Typically with turf toe, the injury is sudden. It is most commonly seen in athletes playing on artificial surfaces, which are harder than grass surfaces and to which cleats are more likely to stick. It can also happen on a grass surface, especially if the shoe being worn doesn’t provide adequate support for the foot. Often the injury occurs in athletes wearing flexible soccer-style shoes that let the foot bend too far forward.
What Are the Symptoms of Turf Toe?
The most common symptoms of turf toe include pain, swelling, and limited joint movement at the base of one big toe. The symptoms develop slowly and gradually get worse over time if it’s caused by repetitive injury. If it’s caused by a sudden forceful motion, the injury can be painful immediately and worsen within 24 hours. Sometimes when the injury occurs, a “pop” can be felt. Usually the entire joint is involved, and toe movement is limited.
How Is Turf Toe Diagnosed?
To diagnose turf toe, the doctor will ask you to explain as much as you can about how you injured your foot and may ask you about your occupation, your participation in sports, the type of shoes you wear, and your history of foot problems. The doctor will then examine your foot, noting the pattern and location of any swelling and comparing the injured foot to the uninjured one. The doctor will likely ask for an X-ray to rule out any other damage or fracture. In certain circumstances, the doctor may ask for other imaging tests such as a bone scan, CT scan, or MRI.
How Is Turf Toe Treated?
The basic treatment for treating turf toe, initially, is a combination of rest, ice, compression, and elevation (remember the acronym R.I.C.E).This basic treatment approach is to give the injury ample time to heal, which means the foot will need to be rested and the joint protected from further injury. To rest the toe, the doctor may tape or strap it to the toe next to it to relieve the stress on it. Another way to protect the joint is to immobilize the foot in a cast or special walking boot that keeps it from moving. The doctor may also ask you to use crutches so that no weight is placed on the injured joint. In severe cases, an orthopaedic surgeon may suggest a surgical intervention.
It typically takes two to three weeks for the pain to subside. After the immobilization of the joint ends, some patients require physical therapy in order to re-establish range of motion, strength, and conditioning of the injured toe.